Nutrition and Falls Risk
Falls are a major cause of injury in older people. According to the National Falls Prevention Plan for Older People, people over the age of 65 are at a greater risk of sustaining an injury from a fall. The risk of falls is not equal for all individuals of the same age, however, due to a range of factors including eyesight, balance, muscle strength, bone density and medications taken.
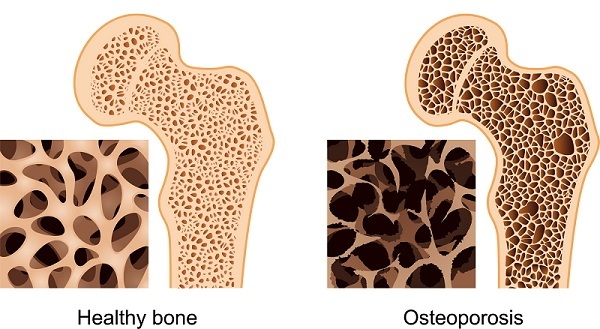
Bone Density and Osteoporosis
Osteoporosis is a common bone disorder that causes a progressive loss in bone density and mass. Osteoporosis is often called a ‘silent disease’ because it usually has no signs or symptoms until a fracture occurs. In fact, in Australia 1 in 2 women and 1 in 3 men over the age of sixty will have an osteoporotic fracture.
From early adulthood, bones gradually begin to lose mineral, density and strength. Factors that help to reduce the rate of bone loss and the risk of osteoporosis include limiting alcohol, not smoking, regular weight-bearing exercise, eating plenty of calcium rich foods and getting adequate vitamin D.
Throughout the life cycle, calcium and Vitamin D play an important role in bone health. Both men and women lose bone mass as they age. The need for additional calcium for older Australians is reflected in the national dietary guidelines.
Vitamin D
Despite living in sunny Australia, recent studies have shown that a significant number of Australians suffer from vitamin D deficiency. This is particularly prevalent for higher risk groups including the elderly, those who are housebound, people who cover up for religious or cultural reasons and people with darker skin tones.
Vitamin D helps to regulate the amount of calcium in the blood and essential for calcium absorption into the bones. It also plays a role in muscle strength. Low vitamin D status increases the risk of osteoporosis and weaker muscles, leading to a higher chance of falls. Research indicates that Vitamin D may also play a role in maintaining a healthy immune system, and in protection against respiratory infections, diabetes, depression, multiple sclerosis, inflammatory bowel disease, bowel cancer, breast cancer and prostate cancer.
Although vitamin D can be found in some foods such as oily fish and eggs, the majority of Vitamin D comes through exposure of the skin to the Ultra Violet (UV) rays from the sun. (It is sometimes referred to as the ‘sunshine vitamin’).
Further studies are being conducted to determine exactly how much sun exposure Australians need, but the current recommendation from Osteoporosis Australia states that ‘to get enough sunlight to produce vitamin D, older people needs to expose their hands, face and arms (around 15% of body surface) to sunlight for about 6-8 minutes, 5-6 times per week (before 10am or after 2pm Standard Time in summer, for moderately fair people).’
In Residential Aged Care Facilities (RACFs), it is not always possible for the frail and elderly to have regular exposure to the sun. A blood test can determine serum levels of vitamin D and, if required, appropriate supplementation can be prescribed by a doctor.
Calcium
Calcium is vital for healthy teeth and bones. It also plays a role in the healthy functioning of nerves and muscles. The best sources of calcium in the Australian diet are dairy products such as milk, yoghurt, and cheese and calcium fortified milk alternatives e.g. soy milk. Dairy foods also contain other important nutrients essential for bone health including protein, phosphorus, magnesium and zinc. Alternative sources of calcium include canned salmon and sardines (eaten with the bones), green leafy vegetables, some nuts, cereals and legumes. These foods contain smaller amounts of absorbable calcium than dairy foods.

Other factors that may affect falls risk include malnutrition, dehydration, nutritional deficiencies and physical activity.
Malnutrition
Malnutrition is a significant issue for older Australians. Malnutrition is a condition resulting from inadequate dietary intake or impaired digestion of nutrients. One of the consequences of malnutrition is increased risk of fracture due to poor bone density and increased risk of falls due to muscle weakness.
In hospitals and RACFs, Nutrition Screening can help to identify those at risk before they become malnourished. Residents should be screened on admission and at regular monthly intervals thereafter.
Dehydration
Dehydration increases an individual’s risk of falls. Dehydration can lead to confusion, dizziness, a loss of muscle tone, drowsiness, decreased reaction time and postural hypotension. Ensure that individuals have adequate access to fluids, at least 1500ml per day (unless requiring a fluid restriction). Fluids include water, milk, tea, coffee or juice. If residents require thickened fluids, ensure they are prepared to the appropriate texture and provided with assistance and encouragement as necessary.

Nutrient deficiencies
Nutrient deficiencies may increase risk of falls due to the symptoms they result in.
Iron, for example, plays a role in transporting oxygen around the body and is essential for a strong immune function, muscle strength and good mental function. Iron deficiency can lead to an increased risk of falls due to fatigue and decreased concentration. If someone has large blood losses or does not eat enough iron rich foods regularly, they may be at risk of iron deficiency. Iron rich foods include: red meats, poultry, fish, eggs, lentils and nuts. There is also some iron found in wholemeal pasta and bread and dark leafy vegetables, but this is not as readily available to our bodies. Iron rich foods should be included regularly across the week.
Note: Iron supplements should only be used under medical supervision.
Physical activity
Muscle mass declines as we get older, however regular activity (especially weight bearing exercise, appropriate for the individual) can assist with maintaining muscle strength and balance, helping to keep bones strong. Close consultation with doctors, physiotherapists or other health care professionals is recommended to create exercise programs that are healthy and safe for individuals.


